Pudendal Neuralgia is a painful neuropathic condition that is caused by inflammation of the pudendal nerve. Triggers for the sensitivity include trauma secondary to childbirth, surgery, cycling, squatting exercises, bio-mechanical abnormalities (e.g., sacro-iliac joint dysfunction, pelvic floor dysfunction), chronic constipation, repetitive vaginal infections and direct falls on the tailbone. Pudendal neuralgia is known in some circles as ‘cyclist’s syndrome’, ‘pudendal canal syndrome’ or ‘Alcock’s syndrome.’
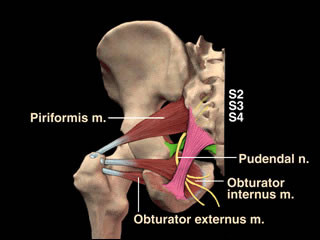
Primary symptoms of Pudendal Neuralgia include:
- Pelvic pain with sitting that may be less intense in the morning and increase throughout the day. Symptoms may decrease when standing or lying down. The pain can be perineal, rectal or in the clitoral / penile area; it can be unilateral or bilateral.
- Sexual dysfunction. In women, dysfunction manifests as pain or decreased sensation in the genitals, perineum or rectum. Pain may occur with or without touch. It may be difficult or impossible for the woman to achieve orgasm. In men, dysfunction presents as pain during erection, difficulty sustaining an erection or painful ejaculation.
- Difficulty with urination / defecation. Patients may experience urinary hesitancy, urgency and/or frequency. Post-void discomfort is not uncommon. Patients may feel that they have to ‘strain’ to have a bowel movement and the movement may be painful and/or result in pelvic pain after. Constipation is also common among patients with pudendal neuralgia. In severe cases, complete or partial urinary and/or fecal incontinence may result.
- Sensation of a foreign object being within the body. Some patients will feel as though there is a foreign object sitting inside the vagina or the rectum.
It is important to note PN is largely a “rule out” condition. In other words, because its symptoms can be indicative of another problem, extensive testing is required to ensure that your symptoms are not related to another condition. Common conditions that should be evaluated include coccygodynia, piriformis syndrome, interstitial cystitis, chronic or non-bacterial prostatitis, prostatodynia, vulvodynia, vestibulitis, chronic pelvic pain syndrome, proctalgia, anorectal neuralgia, pelvic contracture syndrome/pelvic congestion, proctalgia fugax or levator ani syndrome.
In addition to eliminating other diagnoses, it is important to determine if the pudendal neuralgia is caused by a true entrapment or other compression / tension dysfunctions. In almost all cases, pelvic floor dysfunction accompanies pudendal neuralgia. Electrodiagnostic studies will help the practitioner determine if the symptoms are caused by a true nerve entrapment or by muscular problems and neural irritation. It is crucial to a successful treatment outcome to acknowledge both dysfunctions and treat accordingly. In the event of a true entrapment, surgical decompression followed by post-operative physical therapy will be necessary to restore patient health. In cases of pudendal neuralgia, pudendal nerve blocks and physical therapy can alleviate the symptoms and resolve the original problem.
Treatment
Medical
Analgesic medications, even those containing narcotics may have limited efficacy for neuropathic pain. Pain modulators such as tricyclic antidepressants and neuroleptics (i.e. Neurontin, Zonegran, etc.) have varied efficacy. Nerve infiltration with a combination of local anesthetic (Lidocaine or Marcaine) combined with steroid (Triamcinolone or Solu-Medrol) or combined with Heparin can be used. Multiple injections (usually 3-5) may be required. Timing intervals vary but 3-6 week interval between infiltration seems reasonable. Success rates also vary widely where between 15-60% are cured or improved with this approach alone.
Lifestyle Modifications
Avoiding activities which worsen the condition is crucial (cycling, sitting, etc.). Sitting pads, especially those designed with cutouts to transmit pressure away from the perineum, can be very helpful.
Physical Therapy
Musculoskeletal dysfunctions can cause pudendal neuralgia as well as other painful pelvic syndromes. Physical therapy is an effective method of minimizing or eliminating the concurrent pain generators that occur when the pudendal nerve is irritated (i.e., pelvic floor hypertonicity and myofascial trigger points, extrapelvic hypertonicity and trigger points, adverse neural tension, sacro-iliac joint dysfunctions, connective tissue restrictions, and faulty neuromuscular recruitment patterns). It is important to acknowledge this interaction between musculoskeletal and neural dysfunction as it is unusual that one exists without the other.
Physical therapists require special training to treat pudendal neuralgia. The therapist should have a strong manual therapy bias and an extensive working knowledge of pudendal neuralgia. The program should emphasize restoring normal length to the pelvic floor (through internal myofascial release) and pelvic floor relaxation techniques. Typically, the shortened pelvic floor/pudendal neuralgia will become symptomatically exacerbated with Kegel exercises and these should be avoided until otherwise instructed by a professional. The program should also include connective tissue mobilization, neural mobilization and a home exercise program.
Surgical
Three main surgical techniques are currently available (worldwide) for nerve decompression. The theory is similar to other nerve decompression procedures performed for nerve entrapments in other regions of the body (i.e. carpal tunnel release). The procedures differ in their approach to the area of entrapment and have never been compared head to head.
Post-Operative Physical Therapy
The above mentioned musculoskeletal dysfunctions can be responsible for pain that persists after a decompression procedure. It is recommended that external physical therapy begin one month post-operatively and that pelvic floor rehabilitation gets initiated at three months.
Sacro-iliac joint dysfunction commonly co-exists with pelvic pain. When the sacrotuberous ligament is severed during decompression, SIJD is a common post-operative complication. Patients typically will have persistent (or ‘new’) pain and pelvic dysfunction. This situation is correctable through proper stabilization techniques: through physical therapy in less involved circumstances and through proliferative therapy and physical therapy in more severe circumstances.
